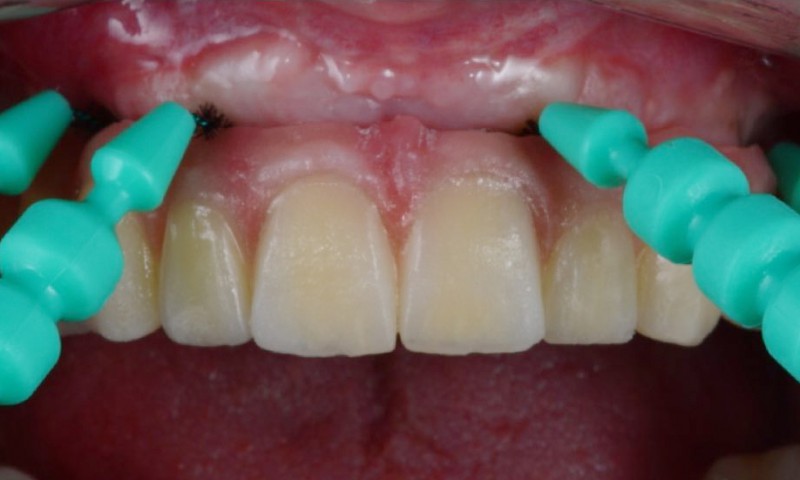
Dental implants have significantly improved the rehabilitation of partially or totally edentulous patients. Nevertheless, implants, like natural teeth, are not immune to mechanical and biological complications.
Peri-implant diseases are becoming increasingly common in dental patients. Several studies have reported alarming rates of mucositis and peri-implantitis. A recent systematic review (1) reported findings of mucositis in 63.4% of patients and 30.7% of implants, and peri-implantitis in 18.8% of patients and 9.6% of implants.
There are a number of risk factors, with varying levels of scientific evidence, for progression of peri-implant diseases, including poor oral hygiene, smoking, diabetes, genetic predisposition, factors associated with the design and position of abutments and crowns, etc. Plaque, however, is the principle and, more importantly, the most effectively treated aetiological factor.
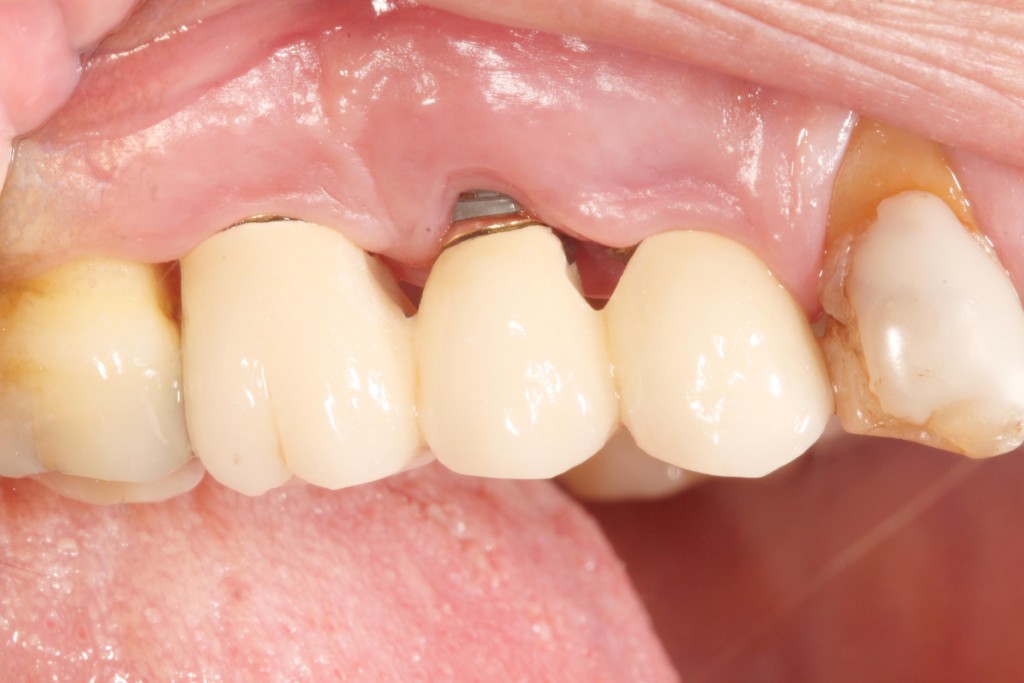
Patient information and disease prevention by means of good plaque control and periodontal check-ups are essential to prevent onset of these pathologies. Only 50% of surgical intervention for peri-implantitis is successful in the long-term (2), even though it is currently the most effective treatment. This strongly suggests that prevention based on a strict implant maintenance protocol is the best way to prevent onset of these diseases.
Poorly designed implants can sometimes limit access to the piece, thus preventing appropriate oral hygiene and facilitating onset of peri-implant diseases. A study (3) in patients with clinical signs of peri-implantitis reported that 74% of implants were not accessible for adequate plaque control, and 48% of these presented peri-implantitis. Of the remaining implants, 26% had good access for hygiene, and only 4% of these presented peri-implantitis.
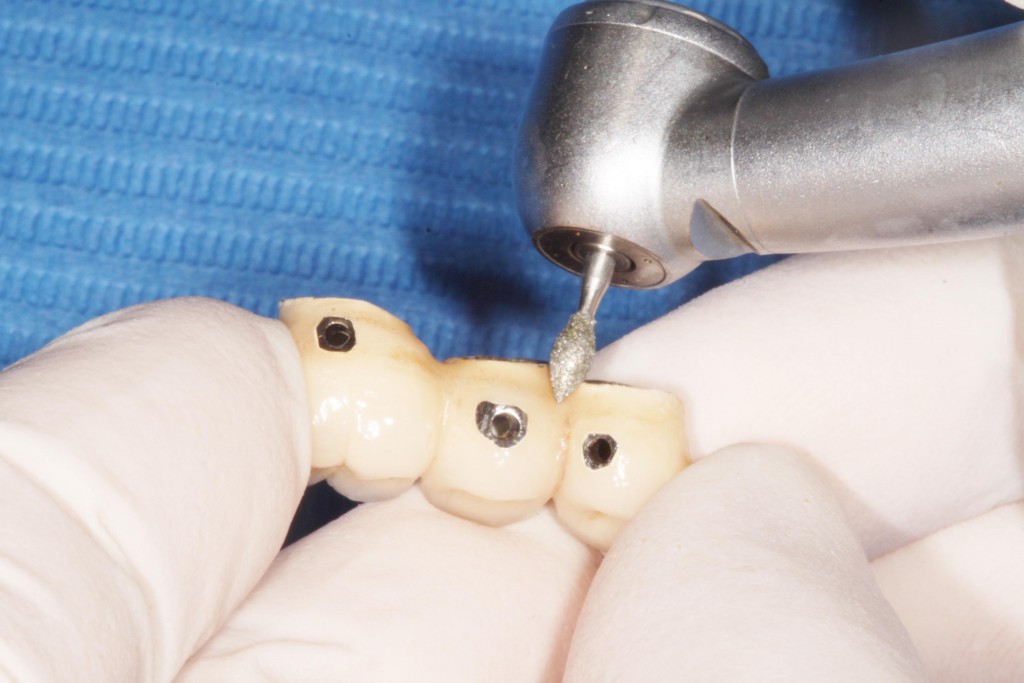
It is important, therefore, to establish a periodontal re-evaluation and maintenance protocol to be followed both in the dental clinic and at home by the patient. (4)
-
- PREVENTION. Explain to patients the type of abutment and crown they will receive before proceeding with implantation. Make sure they have evaluated the risk factors and understand the importance of maintenance following final rehabilitation, and offer alternative treatment options.
-
- INFORMATION. Give patients informative brochures and show them photos and models to explain what their implant will look like and how they must care for it. It is important that patients understand that sometimes ensuring access for hygenic purpose will take priority over aesthetic considerations.
-
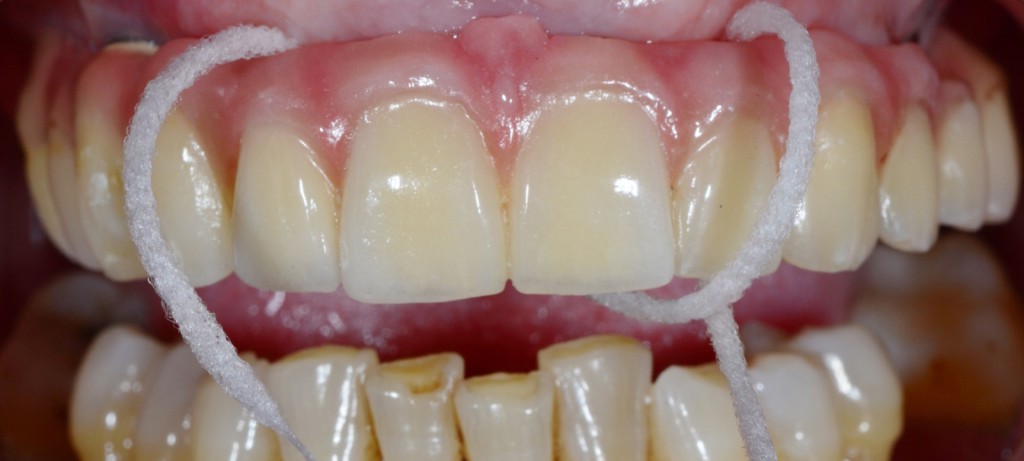
- TEACH ORAL HYGIENE AND BIOFILM CONTROL TECHNIQUES. Teach patients the specific oral hygiene techniques they will need to care for their particular implant. It is important that patients know how to access all their implants for adequate biofilm management.
-
- RE-EVALUATION AND CHECK-UPS. Check the status of all implants at each visit by evaluating bleeding and taking probe measurements. If changes in pocket depth and bleeding occur, take follow-up x-rays and compare them with the baseline images taken on the day the implant was fitted.
-
- MOTIVATION. Take advantage of each periodontal check-up to motivate patients to prevent the onset of peri-implant disease. Always be positive and encouraging.
-
- ACTIVE TREATMENT. In the clinic, always monitor biofilm status and repeat oral hygiene instructions. Recommend the use of electric tooth brushes, interdental brushes, special dental floss and single-tuft brushes. For mechanical debridement, use instruments that will not damage the surface of the implant or the prosthesis. Metal and titanium curettes and ultrasound scalers damage the abutment and the neck of the implant (5). It is better to use carbon fibre, teflon or plastic instruments or rubber cups that can remove plaque and calculus with damaging these structures. In implants with poor access, consider modifying the crown and disassembling it to gain access for debridement. Antimicrobials such as chlorhexidine gel are used as an adjunct to mechanical debridement to prevent bacterial re-colonisation, and as an oral hygiene aid for patients. Finally, advise patients to use their oral hygiene protocol at least twice a day, and agree on a 3- or 6-monthly periodontal check-up schedule.
References
-
- Atieh MA, Alsabeeha NH, Faggion CM Jr, Duncan WJ. The frecuency of peri-implant diseases: asystematic review and meta-analysis. J Periodontol. 2013 Nov;84(11):1586-98.
-
- Serino G, Turri A. Outcome of surgical treatment of peri- implantitis: results from a 2-year prospective clinical study in humans.
Clin. Oral Impl. Res. 22, 2011; 1214–1220.
-
- Serino G, Stro ̈m C. Peri-implantitis in partially edentulous patients: association with inadequate plaque control.
Clin. Oral Impl. Res. 20, 2009; 169–174.
doi: 10.1111/j.1600-0501.2008.01627.x
-
- Figuero E, Graziani F, Sanz I, Herrera D, Sanz M. Management of peri-implant diseases. Periodontology 2000, Vol. 66, 2014, 255–273
-
- Matarasso S, Quaremba G, Coraggio F, Vaia E, Cafiero C, Lang NP.Maintenance of implants: an in vitro study of titanium implant surface modifications subsequent to the application of different prophylaxis procedures. Clin Oral Implants Res. 1996 Mar;7(1):64-72.