

INTRODUCTION
Oral rehabilitation with implant-supported prostheses is, without doubt, the best rehabilitation treatment available today. Studies with more than 25 years of follow-up have shown the survival and success rate of this type of treatment. However, the number of cases of mucositis and periimplantitis found in clinical practice is steadily increasing. Although prevalence of these diseases range from 4.7% to 36% of implants, depending on the study consulted, all authors are unanimous in pointing out the steady rise in the number of cases.
The success of an implant depends not only on correct insertion in the bone tissue, but also on maintaining the integrity and health of all the tissues involved in the process. This is why good hygiene, patient training, motivation and control are key to prolonging the life of implants.
IMPLANT MAINTENANCE PROTOCOL
It is important to establish a good follow-up protocol for monitoring patients with implants. Creating a decision-making algorithm and establishing the check-up schedule are the key to saving valuable consultation time, and will allow us to create a simple routine that can be followed by all members of the team.
The first step is a visual inspection of the peri-implant tissues, noting all relevant parameters in the patient’s file:
• The presence, quantity, and location of calculus deposits. These can be evaluated using same indexes used for natural teeth.
• Examine mucosa and connective tissue, looking for changes in colour, contour, or consistency of the mucosa, without forgetting that intra-alveolar tissue, which is more reddish in healthy gums, can also be present.
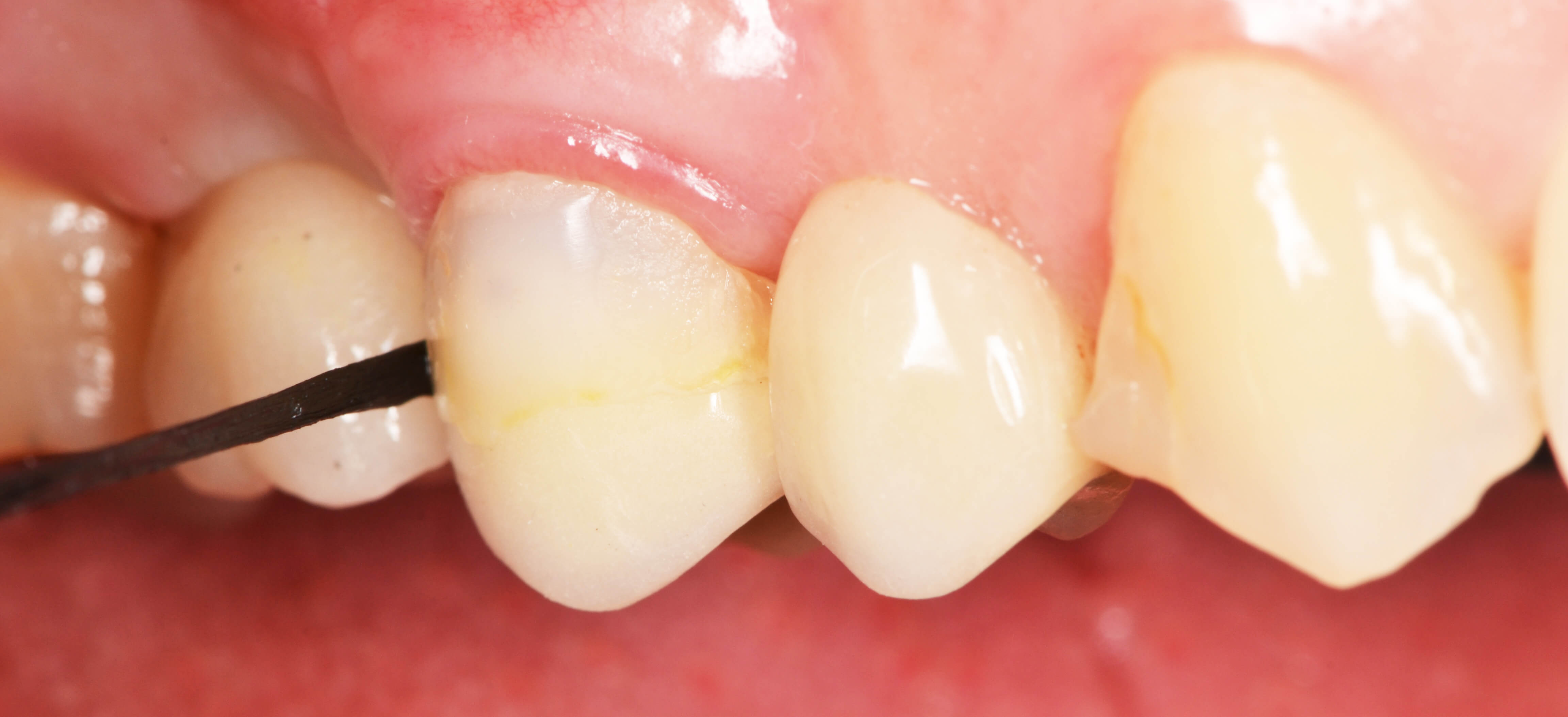
• Probing: Probe depth (PD) is the most widely used measure, although recent studies have shown that increased PD is not always associated with mucositis and periimplantitis. It is also important to remember that in some cases probing is not advisable or may have limited efficacy, either due to poor access or to the type of prosthesis. Probing must be performed with specific plastic or Teflon probes to avoid damaging the surface of the implant and altering the electrochemical relationships that may affect their compatibility. Probing should not be performed in the first 3 months after connection of the transmucosal element. The pressure exerted must be minimal (15N), since damage to the epithelium can occur.
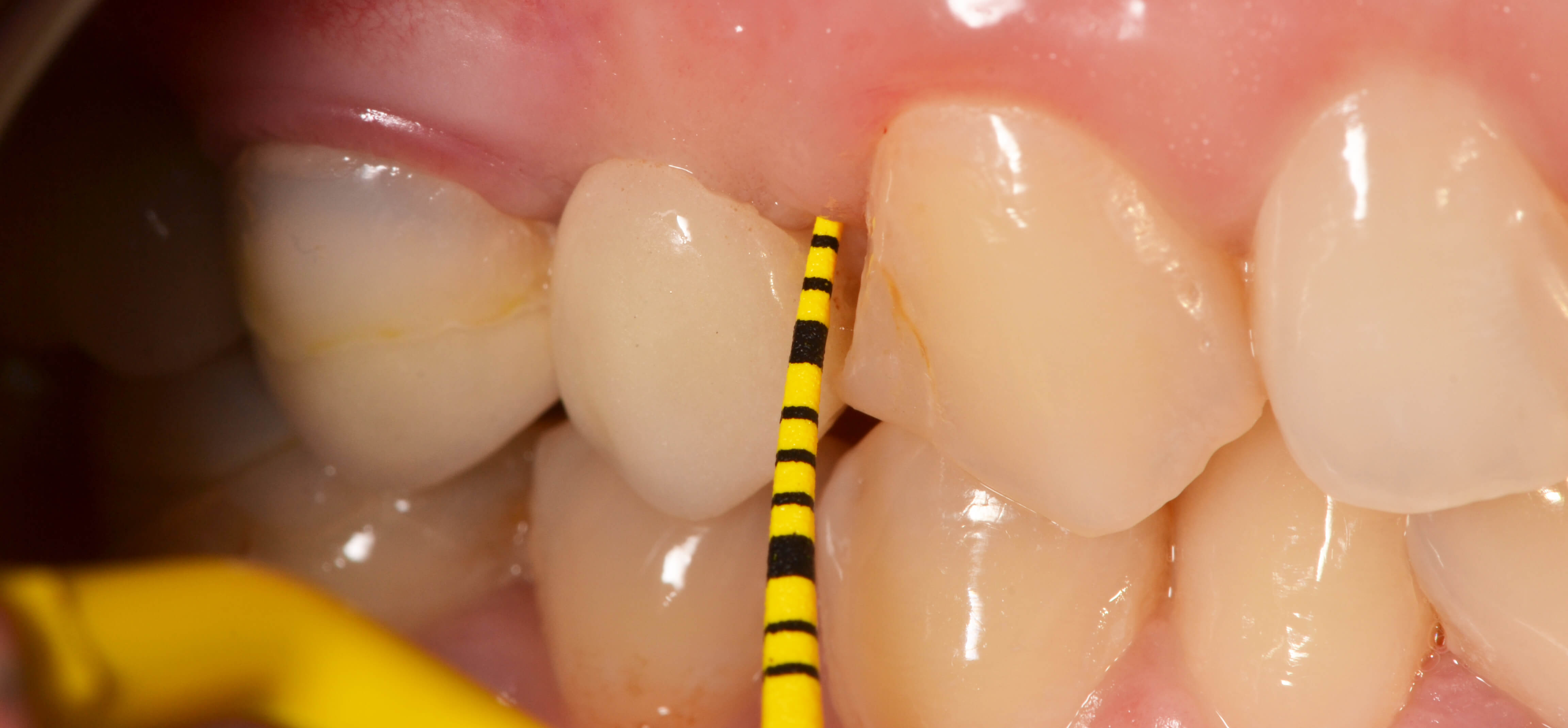
• Bleeding index: It is essential to use this index to quantify bleeding during probing, because prior to onset of periimplantitis, mucositis is characterized by a generalized inflammation of the peri-implant tissue, which will bleed at minimal probing pressure in 100% of patients.
• Radiographic follow-up: essential to assess the loss of hard tissue. Standard long cone paralleling should always be used to ensure all radiographs are identical and can be compared. If no alterations are observed, the x-rays should be taken:
1. When the transmucosal implant is connected.
2. the day the prostesis is placed.
3. Six months after placement of the prosthesis.
4. Anually, for the first 3 years.
5. Every 2 years after the third year.
The prosthesis is as important as the peri-implant tissues. It must be examined for fractures, wear, or the loss of an element, without forgetting mobility, a very important factor that must be taken into consideration. Prostheses supported by several implants should be disassembled annually in order to examine each individual implant.
It is essential to teach patients good oral hygiene habits. As health professionals, we must inform patients that smoking, treatment with bisphosphonates, and decompensated diabetes mellitus are additional risk factors, as tissue healing in this “risk group” can be delayed.
Good motivation can be defined as any incentive that makes the patient commit to their hygiene. The patient must understand that plaque control is the only thing that can optimise the health of their implants. It is mandatory for all professionals to be familiar with the tools available to achieve this goal, and to start patient education even before implant placement:
• Plaque revealing tablets: a visual aid to show patients where they need to focus on brushing.
• Dental floss and dental tape: Available in various thicknesses and types. There is also a black tape that allows patients to clearly see the plaque removed from the interdental spaces.
• Toothbrushes: it is important to know what type of brush to advise in each case. There are also single-tuft brushes specially designed for brushing around the implant.

• Interdental brushes: For brushing between the teeth.
• Toothpaste: it is important to advise patients to use a low-RDA (less abrasive) paste.
• Mouthwashes: especially those that are rich in CPC and provitamin B5. Triclosan, used in many products, is now frowned on, particularly by FDA, due to its bioaccumulative characteristic, and because it is carcinogenic at high concentrations.
• Oral irrigators: these are without a doubt the most useful tools for eliminating the deposits that accumulate under the prosthesis.
• Curettes: plastic, Teflon or even titanium, to respect the surface of the implant.
• Ultrasound: the tips are now often coated with ceramic materials such as PEEK.
It is important to add “implant maintenance” appointments to our daily schedule, protocolising each step in the follow-up procedure and performing each test needed to ensure the success of the restoration. The frequency of check-ups or the need for treatment will depend on the results obtained during these visits. A good way to guarantee success is to establish a decision algorithm that allows us to situate ourselves at the point that corresponds to the patient’s condition, and shows us which steps to take.