
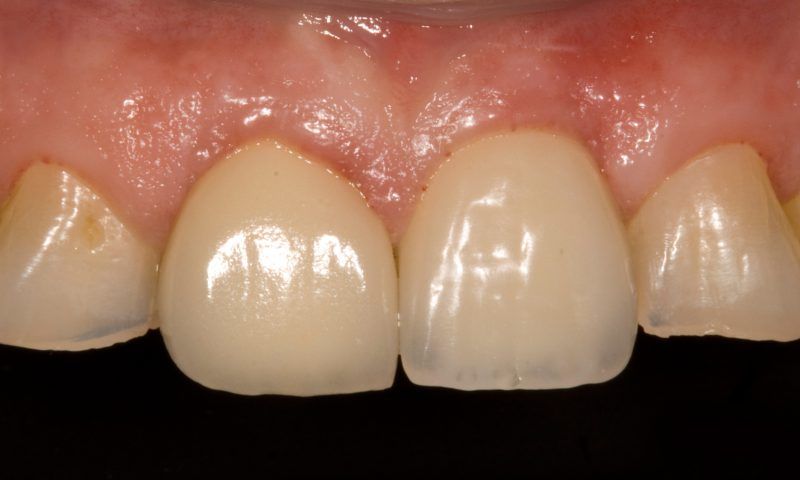
Treatment in the anterior esthetic zone is particularly challenging. The use of immediate temporary abutments makes it possible to reproduce the interproximal spaces and to satisfactorily shape the peri-implant soft tissue.
The literature shows that implants placed during the same surgical operation in which a tooth is extracted have a high success rate.
This technique, combined with good alveolar regeneration treatment, makes it possible to reduce tooth socket bone resorption after the extraction, to shorten the restorative treatment time and to avoid a second surgical operation to place the implant.
Treatment in the anterior esthetic zone is particularly challenging. The use of immediate temporary abutments makes it possible to reproduce the interproximal spaces and to satisfactorily shape the peri-implant soft tissue.
Case description
Female patient aged 57, receiving treatment for high blood pressure and arthrosis, visits the clinic due to the breakage of the central tooth, on which she had a lithium disilicate crown.
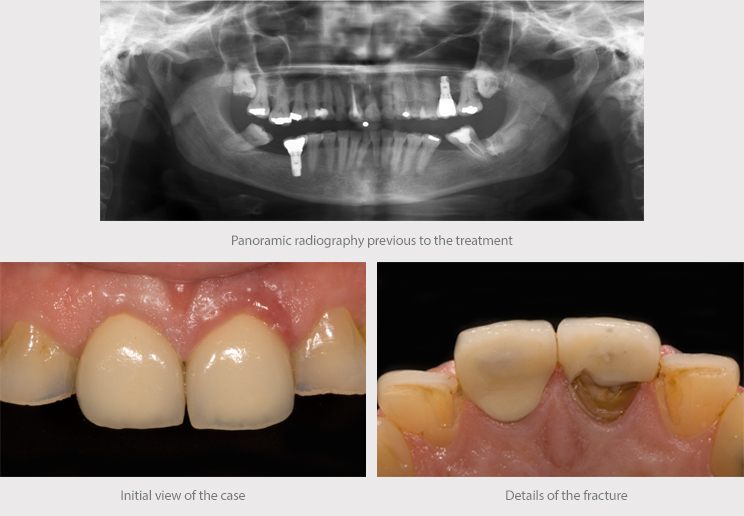
The clinical assessment, using X-rays, clinical photographs and study models, led to a diagnosis and treatment plan suitable for achieving the desired outcome.
The treatment option presented to the patient, with an explanation of the risks and benefits, was an immediate post-extraction implant placement with immediate screw-retained provisionalization and connective tissue graft.
Procedure
The surgery was carried out under local anesthetic. Tooth 21 was extracted with the least possible trauma, respecting the tooth socket walls and with careful curettage to remove any remaining diseased tissue. The state of preservation of the vestibular table was checked and preparations were made for the osteotomy, taking into account the bone type and the recommended drilling sequence for placing a Biomimetic Coral IC implant (4.2 x 13 mm).
The implant was placed using a conventional surgical guide made of acrylic, leaving it below the ridge in the appropriate three-dimensional position for obtaining a good esthetic emergence of the crown. The insertion torque was 45 Ncm, achieving good primary stability, an essential factor in this type of case.
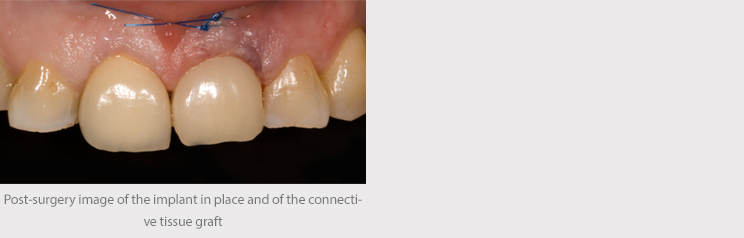
Bone regeneration biomaterial of animal origin (Bio-Oss) was used, as was a collagen plug (Parasorb) to fill the gap between the implant and the vestibular bone wall. During the same surgical operation, connective tissue from the tuberosity was grafted in order to alter the periodontal biotype and thereby improve the prognosis of the treatment.
Immediate nonfunctional loading was then carried out, with an immediate temporary abutment screwed to the implant for six months, which preserved the patient’s appearance during the implant healing period.
It is very important to handle the temporary abutment well in order to achieve satisfactory emergence profiles that can guide and shape the peri-implant tissue prior to the final restoration.
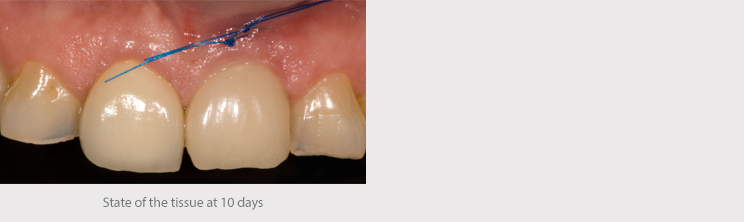
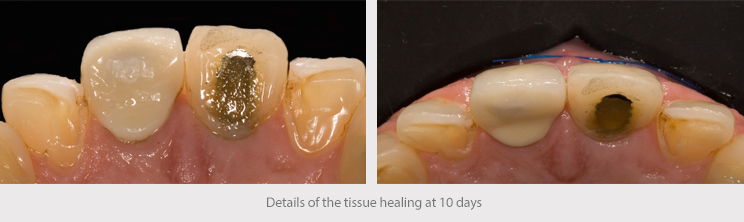
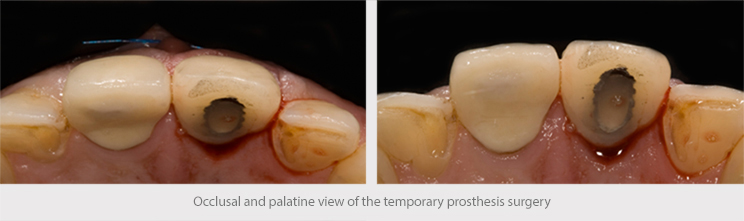 Post-surgery check-ups were carried out at 10, 60 and 90 days.
Post-surgery check-ups were carried out at 10, 60 and 90 days.
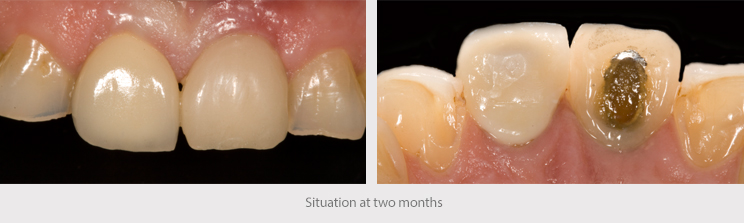 The immediate loading/immediate temporary abutment in post-extraction implants, above all in the anterior region, enables to maintain the gingival architecture and provide support for the connective tissue graft, while also stimulating the alveolar bone through the placement of the implant.
The immediate loading/immediate temporary abutment in post-extraction implants, above all in the anterior region, enables to maintain the gingival architecture and provide support for the connective tissue graft, while also stimulating the alveolar bone through the placement of the implant.
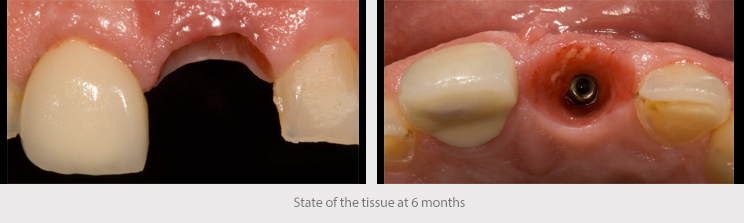
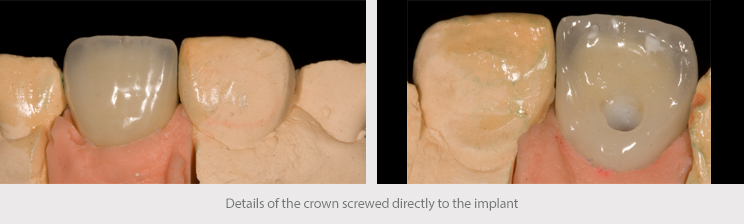
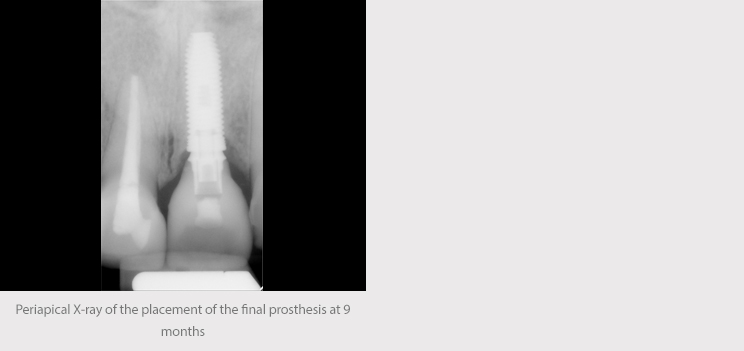 In light of the fact that the patient already had a lithium disilicate restoration on tooth 11, the decision was made to use this material again as the first restorative option in the anterior esthetic zone. A milled crown screwed directly to the implant on a metal interface was made to ensure greater precision and an improved fit.
In light of the fact that the patient already had a lithium disilicate restoration on tooth 11, the decision was made to use this material again as the first restorative option in the anterior esthetic zone. A milled crown screwed directly to the implant on a metal interface was made to ensure greater precision and an improved fit.


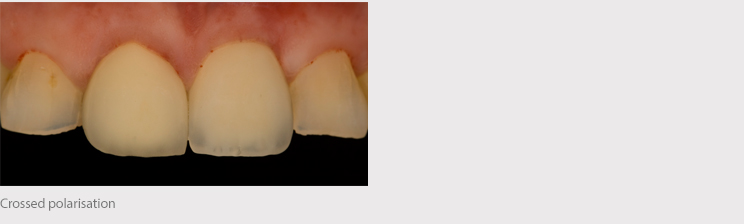
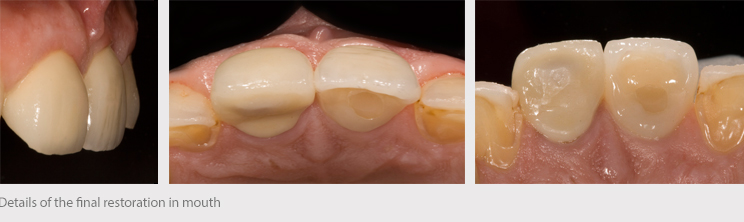
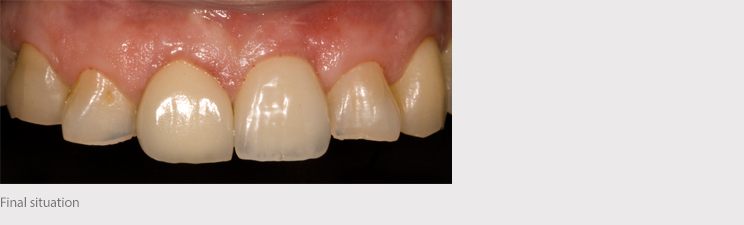
Conclusions
The literature shows that the use of temporary abutments in post-extraction implants with immediate loading, even in the anterior region, is a technique with low morbidity and totally satisfactory functional and esthetic results.
The correct handling of these two techniques is essential and a determining factor in ensuring the success of the treatment and in achieving the patient’s complete satisfaction by fulfilling their expectations.