
By using a connective tissue graft technique, during the implant surgery, different advantages can be achieved such as a suitable thickness and colour of the soft tissue, a fast adaptation of the tissues, a positive tissue architecture, a functionality and aesthetics vital, above all, in the front section.
Introduction
In implant surgery, a good result must be achieved in terms of osseointegration, restoration, functional and aesthetics for the treatment to be correctly defined a success. Therefore, it is very important to study and know the different tissues that will be present in the surgery we are going to perform. As demonstrated in the literature, we know how to handle the bone tissue with a fairly good success percentage; the problem arises in the knowledge and handling of the soft tissue, especially at the time of planning the treatments, since there are few protocols in that regard. One of the major problems we sometimes encounter is soft tissue which is too fine. In these cases, the probability of having tears, implant transparency, etc. greatly increases, and if we also have added bone problems, the complications are multiplied, causing aesthetic alterations that most patients do not accept.
The prevent and treatment of these aesthetic complications are very important. Hence, the transformation of an unfavourable tissue into a favourable one is a vital requirement in order to attain appropriate biological and aesthetic objectives (quantity, quality, texture, colour and gingival biotype), especially if we are treating the anterosuperior oral section.
Protocol
The gingival defects around implants may be mainly due to two aspects: mucogingival defects prior to placing the implants, and which have not been treated before or during surgery, or tissue retractions after the connection of the implant caused by deficient soft tissue and/or bone tissue.
When treatment is being planned, it must anticipate treating this type of complications, and it is necessary to respect the three-dimensional position of the implants to avoid problems with lack of tissue. If this occurs, these defects can often be resolved by mucogingival surgery, returning the necessary dimensions to the peri-implant tissue.
In general terms, for an optimum peri-implant gingival morphology, there must be approximately 20% more tissue than the volume considered necessary. This excess tissue will allow the prosthodontist to adapt the gum to the reconstruction of the prosthesis and achieve the desired aesthetic effects.
This mucogingival intervention may be performed at different points of the treatment:
Currently, the approaches suggest that mucogingival surgeries can only be connective tissue grafts, or be accompanied with reconstructive procedures with guided bone regeneration techniques depending on the quantity of adjacent bone lost. The perpendicular flaps associated to the connective tissue graft are very valid alternatives and with very good aesthetic results that satisfy patients’ requirements.
Presentation of clinical cases – Caso clínico 1
We have a first clinical case of a 38-year old patient, non-smoker and with poor oral hygiene, who came to the surgery due to a small inflammation of the papillae beside the side tooth.
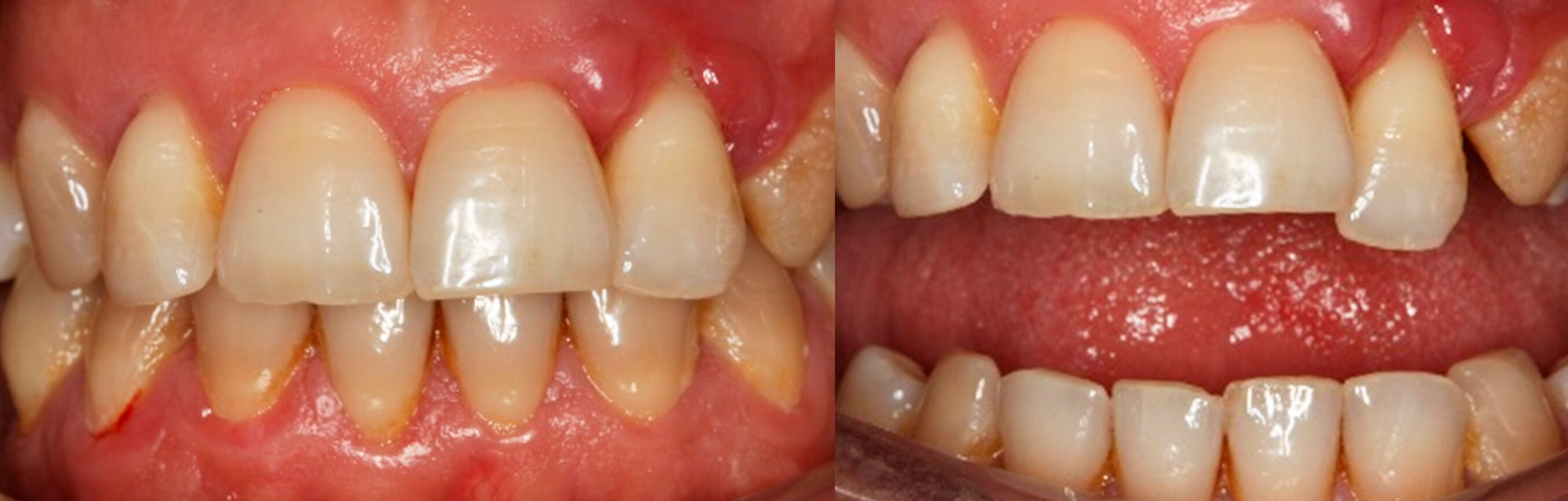 1. Initial image of the case | 2. Patient’s actual situation
1. Initial image of the case | 2. Patient’s actual situation
In the intraoral examination grade, 3 mobility was observed of tooth 22 and the subsequent CAT confirmed the absence of bone around this tooth.
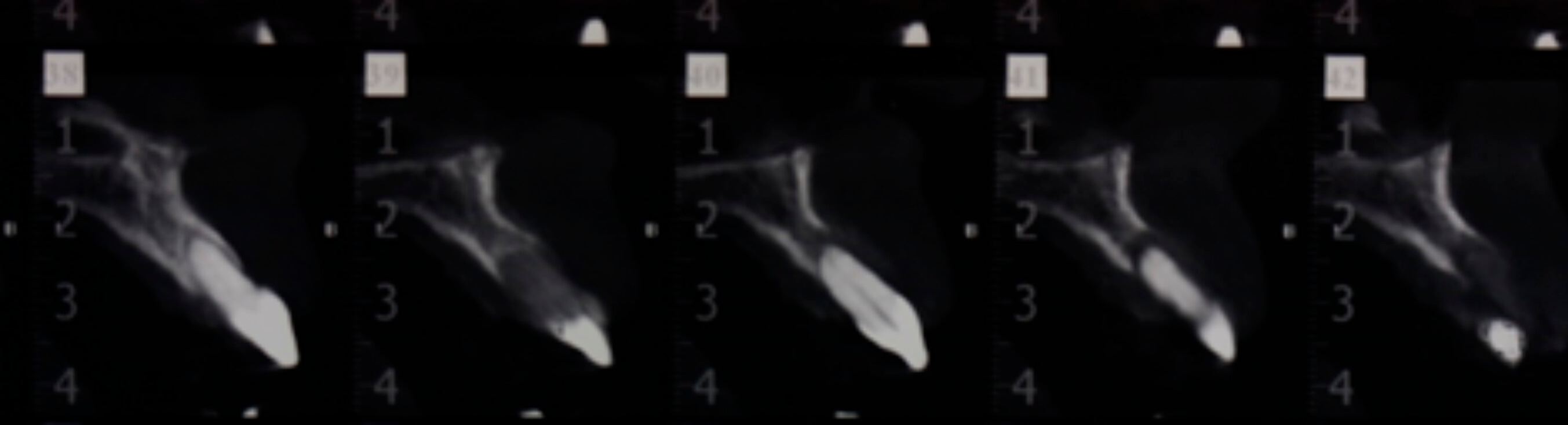 3.Pre-ooperatory CAT
3.Pre-ooperatory CAT
It was decided to remove the tooth and perform curettage on the granulation tissue, which revealed a large vertical and horizontal bone defect.
The proposed treatment plan was to regenerate the defect in a first surgery, with particulate bone (OsteoBiol Apatos, Osteògenos) and a collagen membrane (Osteobiol Evolution, Osteògenos). Furthermore, a soft tissue graft was performed to increase the volume of the vestibular area of the implant, and thus re-establish the peri-implant health, in addition to starting to condition the tissues with a Maryland temporary prosthesis.
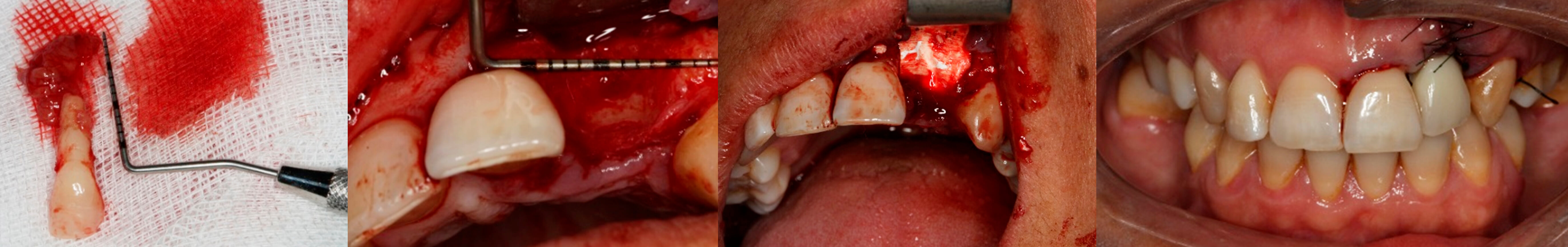 4. Extracted tooth | 5. View of the bone defect | 6. Regeneration detail | 7. Post-surgical image
4. Extracted tooth | 5. View of the bone defect | 6. Regeneration detail | 7. Post-surgical image
The patient was given an appointment after three months to insert a Biomimetic Ocean IC (Avinent) implant (4×11.5mm) and an immediate prosthesis screwed to the implant.
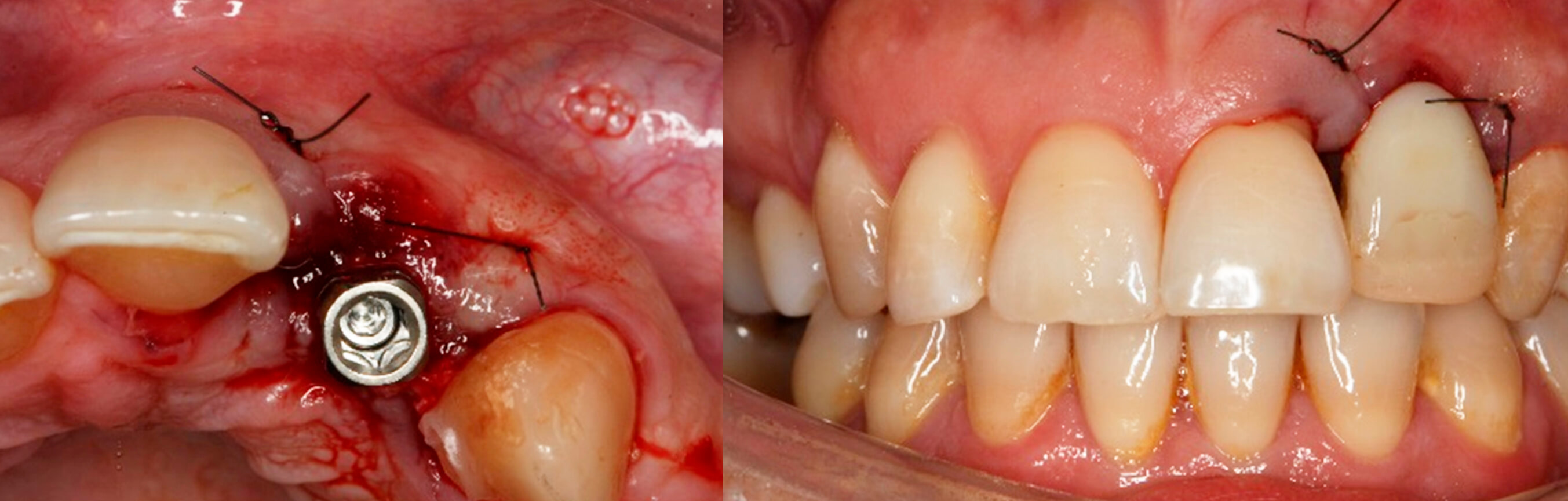 8. Placed implant | 9. Detail of the immediate prosthesis screwed to the implant
8. Placed implant | 9. Detail of the immediate prosthesis screwed to the implant
After verifying good healing of the tissues after 2 weeks, a second mucogingival surgery was decided on to fully achieve the desired aesthetic appearance.
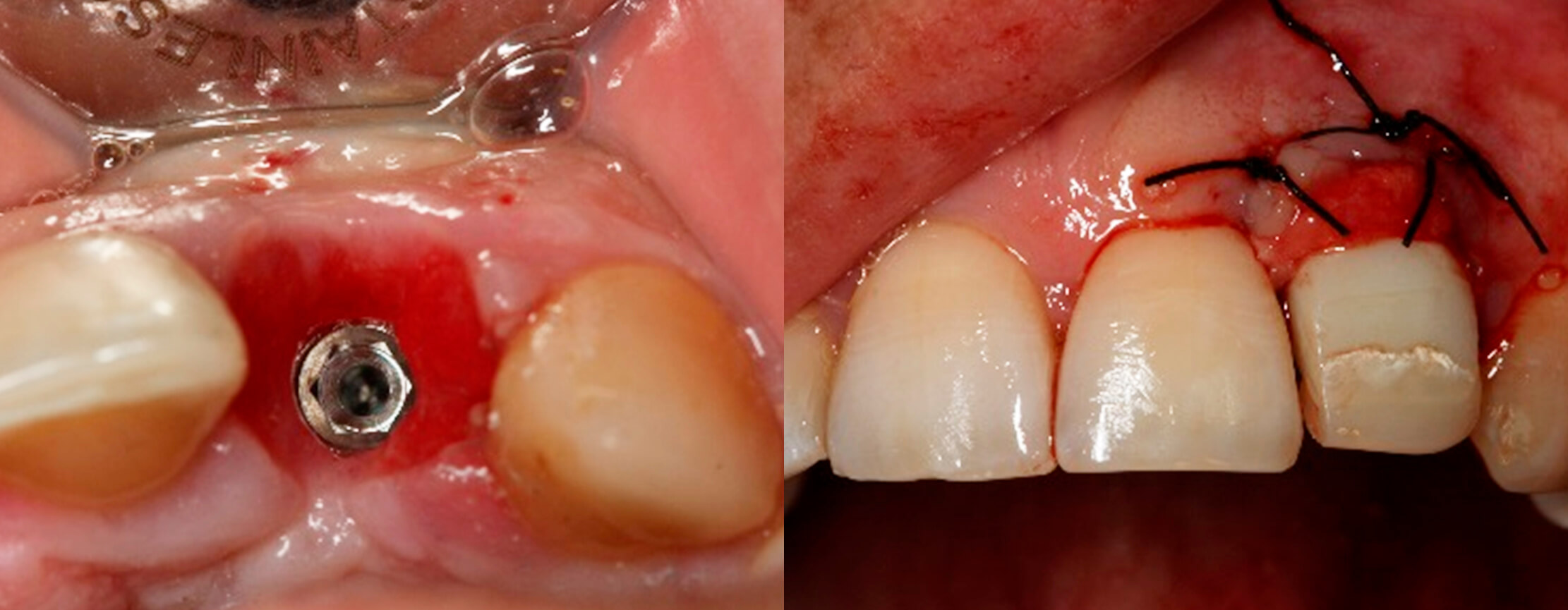 10. Tissue healing after two weeks | 11. Second connective tissue graft
10. Tissue healing after two weeks | 11. Second connective tissue graft
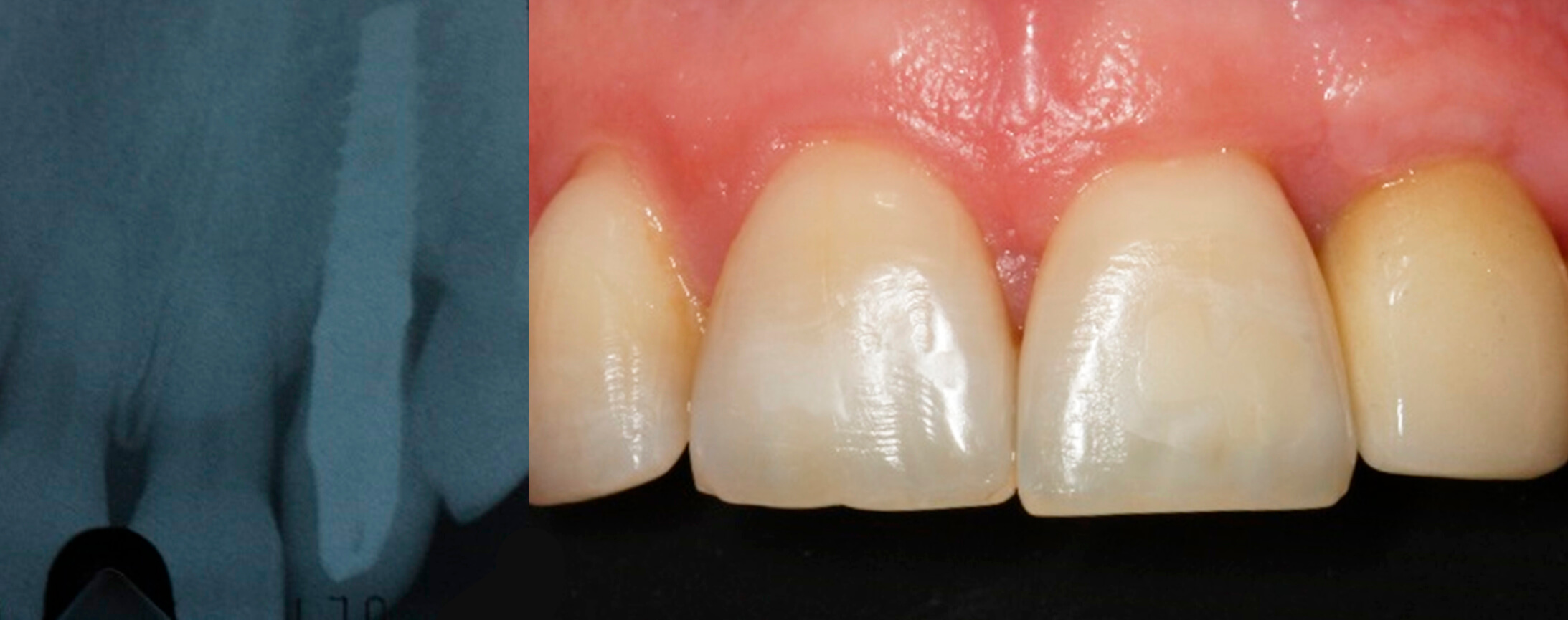 12. X-ray after three years | 13. Situation after three years
12. X-ray after three years | 13. Situation after three years
Presentation of clinical cases – Caso clínico 2
This second case is a 30-year old patient, non-smoker and with good oral hygiene. Due to an accident she attended the surgery with a fracture of root 11 and the incisal edge of 21.
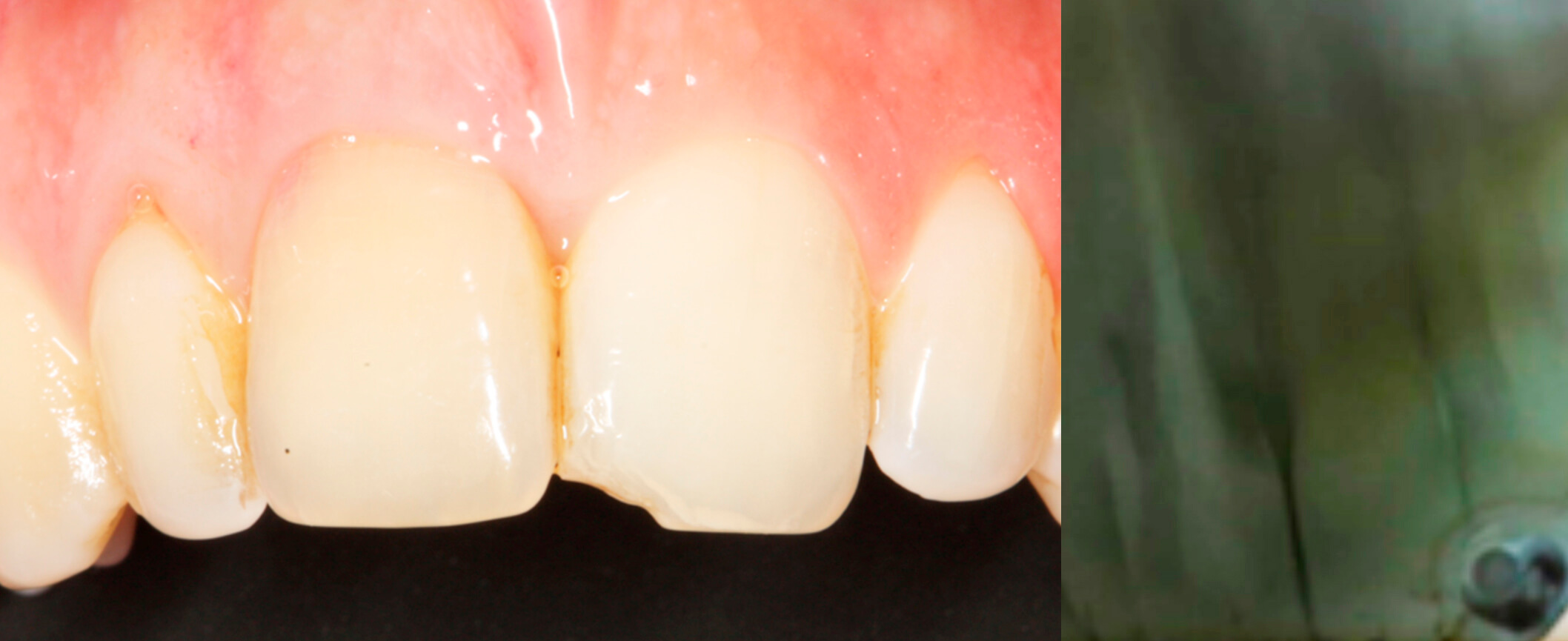 1.Pre-surgical situation | 2. X-ray of the fracture of tooth 21
1.Pre-surgical situation | 2. X-ray of the fracture of tooth 21
The tooth and the root fragments were extracted with great care and a Biomimetic Ocean IC (Avinent) post-extraction implant (4.0×11.5mm) was placed in the same surgery and the alveolar gap was filled with biomaterial (Osteobiol putty, Osteògenos). Since the implant had good stability, an immediate temporary crown was screwed on the same day of the surgery.
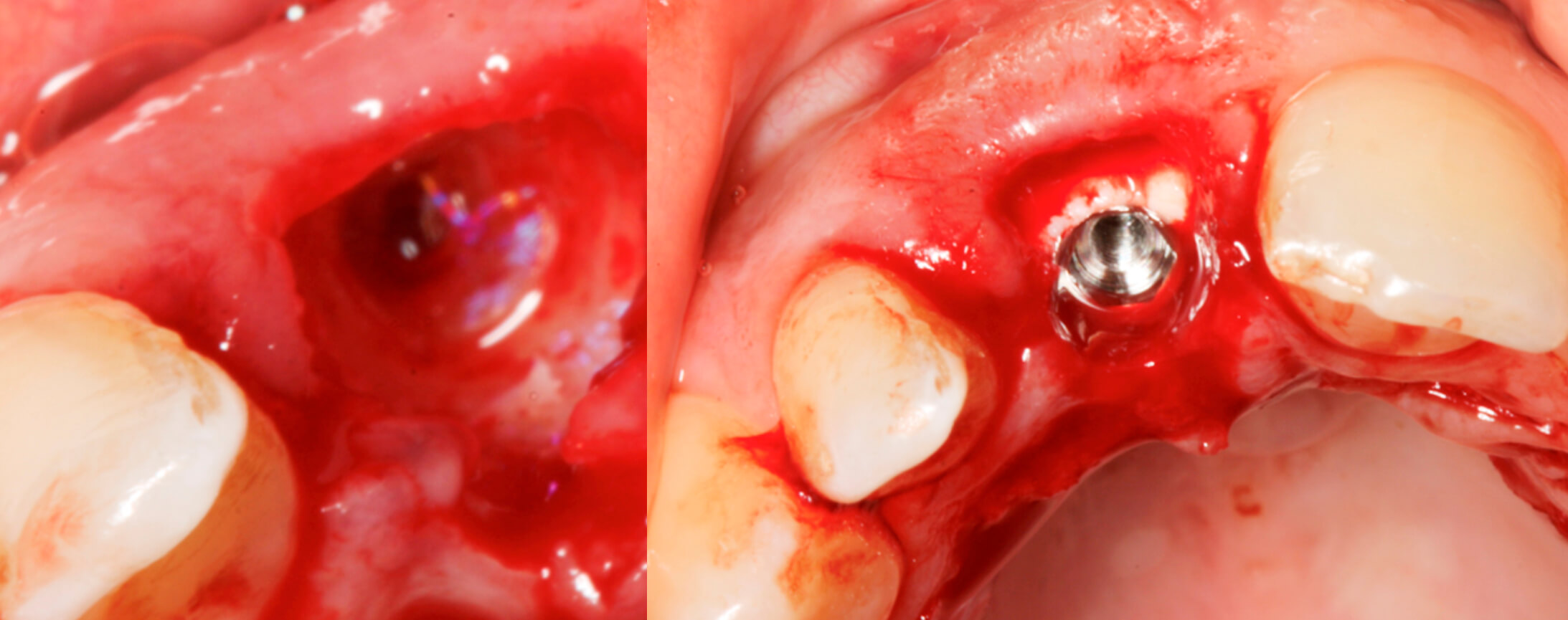 3. Detail of the extraction | 4. Image of the implant immediately post-extraction
3. Detail of the extraction | 4. Image of the implant immediately post-extraction
Good tissue healing was observed after two weeks and it was decided to perform a connective tissue graft with pouch technique using a 5/0 suture.
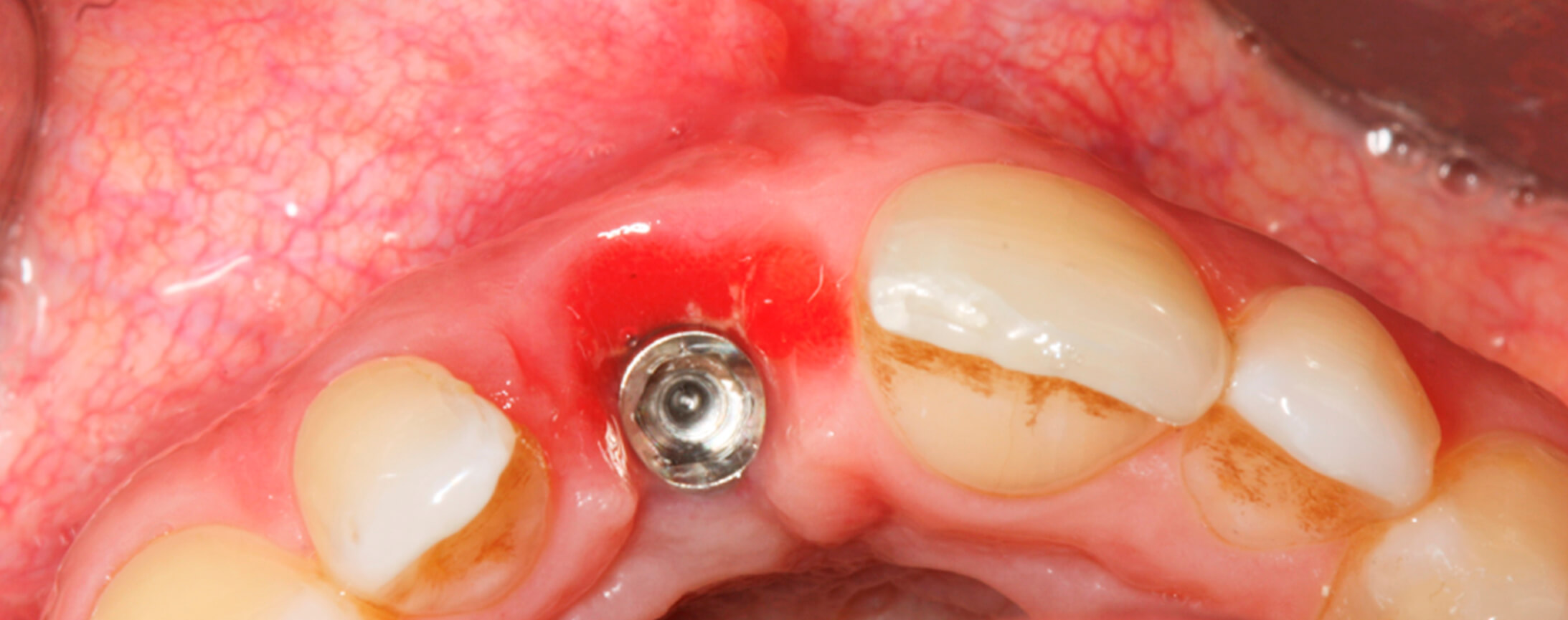 5. Tissues after two weeks
5. Tissues after two weeks
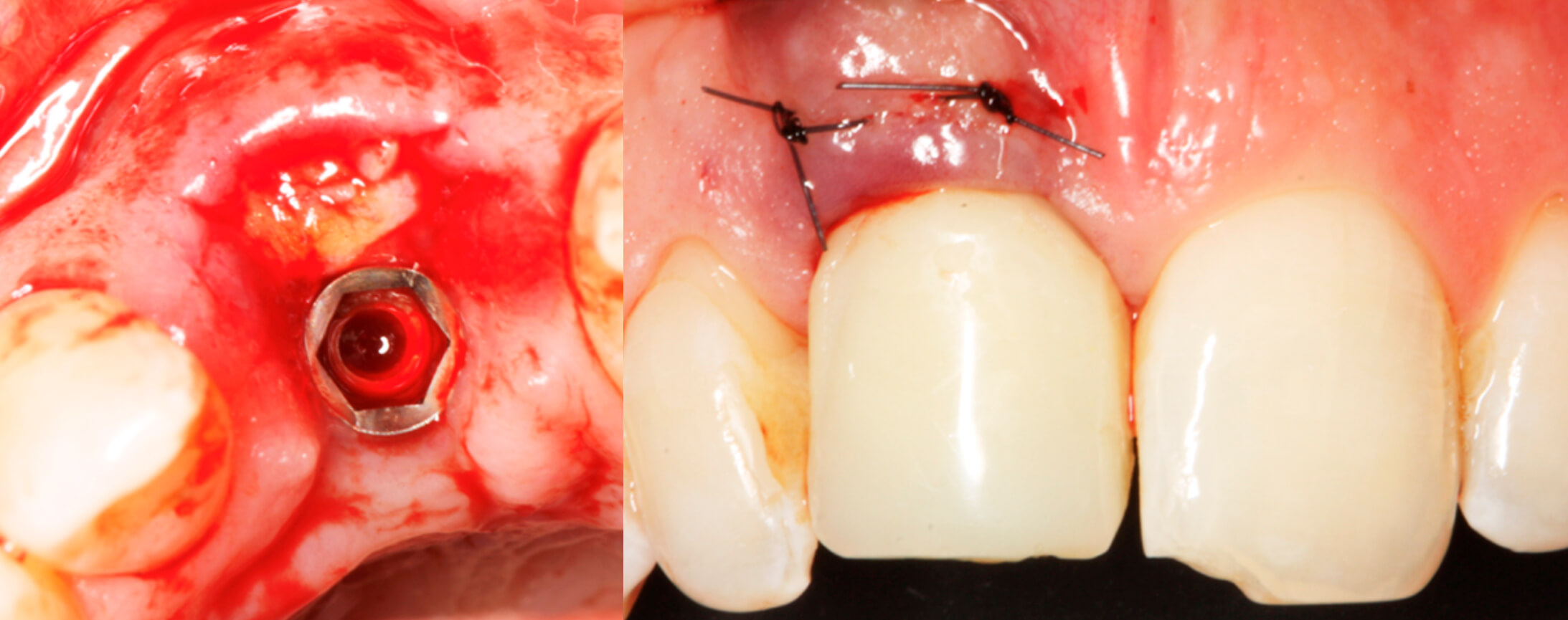 6 y 7. Image of the connective tissues graft pouch technique
6 y 7. Image of the connective tissues graft pouch technique
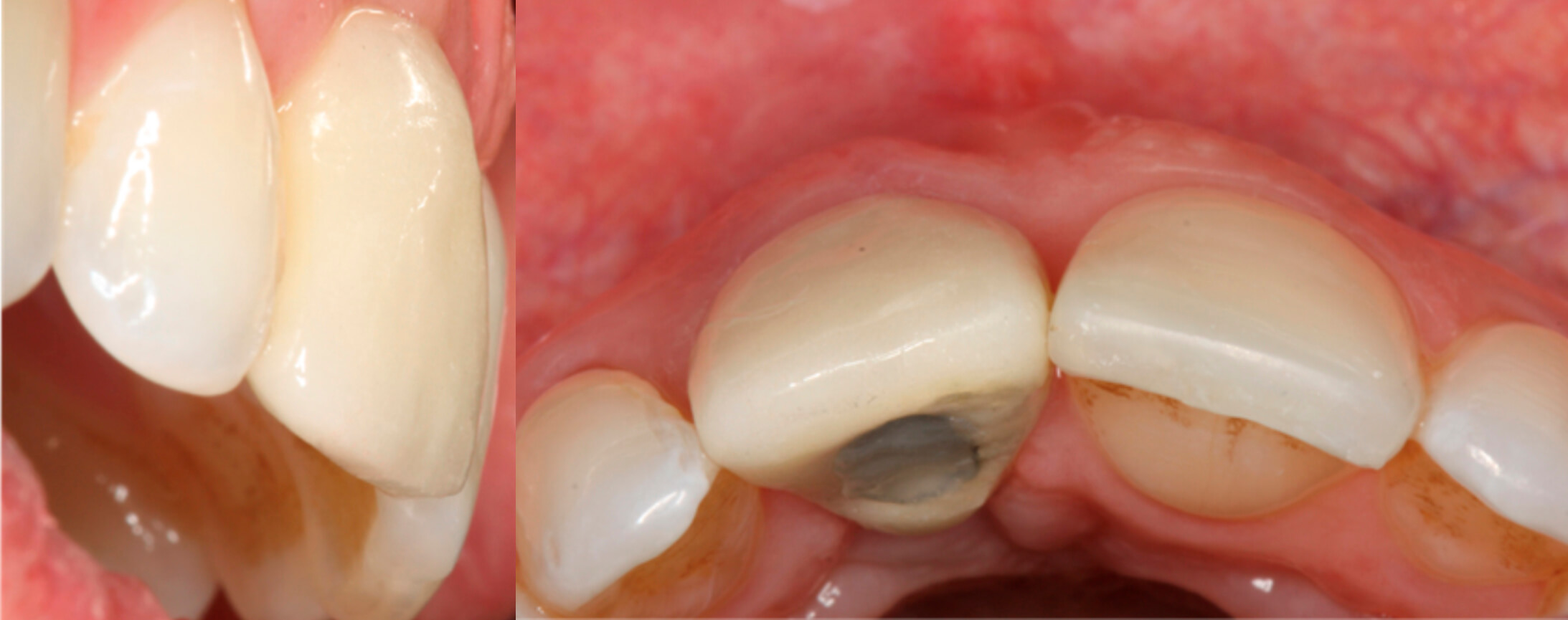 8. Views of the final result
8. Views of the final result
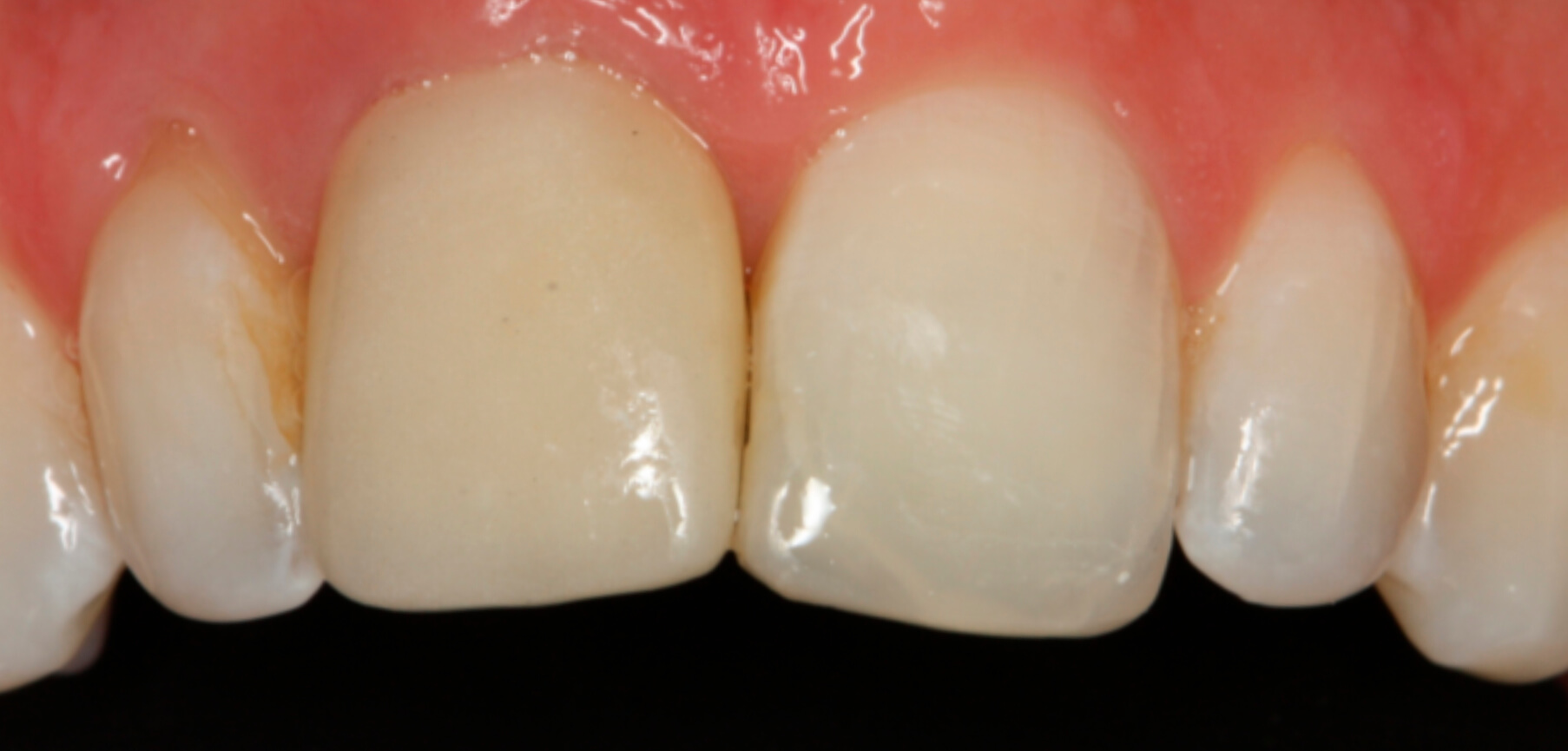 9. Predictable result after three years
9. Predictable result after three years
Conclusión
The great importance of the peri-implant soft tissues is known for the predictability of the treatment with dental implants. By using a connective tissue graft technique, during the implant surgery, different advantages can be achieved such as a suitable thickness and colour of the soft tissue, a fast adaptation of the tissues, a positive tissue architecture, a functionality and aesthetics vital, above all, in the front section.
Biobliografía